Celiac disease is mostly known for affecting the gut health of someone with the autoimmune disease. But did you know that it actually can affect almost all other systems in the body as well? One of which being oral health, thankfully I personally have only experienced a few of these symptoms thus far, I will talk more about this down below.

What are the symptoms of oral health and celiac disease?
- Children and Celiac Disease
This is commonly seen in their permanent teeth rather then baby teeth. The first sign to look out for is they may not have enough enamel, as their teeth may look patchy or discoloured, this is also known as enamel hypoplasia and can cause tooth cavities or an increased tooth sensitivity. A child with celiac disease could also have teeth that are pitted or have a deep horizontal groove.
Children are not the only ones who can have these defects, it can also be seen in adults who have a genetic disorder, poor nutrition or are taking certain medications. Regardless, people with celiac disease are more likely to develop enamel defects then people without the condition. - Enamel Defects
A few theories as to why adults and children can have enamel defects comes to mind. One of which being the nutrition deficiencies that can be caused with celiac disease, or the immune system of the individual is attacking the enamel itself causing the defects.
There have been studies to show that there may be direct immune system damage occurring where dental enamel defects are also found in close relatives of someone with celiac disease but who have not been diagnosed with the condition themselves.
Unfortunately, the damage caused to the enamel is not reversible, however, the dental community has advanced ways of improving peoples mouths these days that are very impressive. - Cavities
This can be common in people who have been or not yet been diagnosed with celiac disease. Sometimes people complain of bad breath with multiple cavities. If there are any enamel defects that has started from childhood or even as an adult, this can lead to cavities occurring, especially with undiagnosed celiac disease.
Due to the damaged caused in the small intestine from active celiac disease, malabsorption of essential vitamins and minerals such as vitamin D and calcium can occur. These are both essential for strong bones and overall good health, not just in the mouth. This can all be resolved for someone with celiac disease to prevent further damage while following a strict gluten free diet. - Mouth Sores or Canker Sores
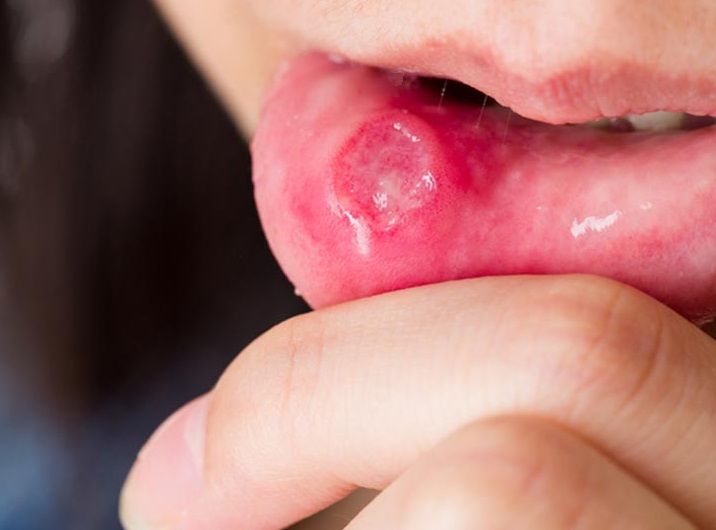
Personally, this was a symptom that I struggled with, I would always have sores in my mouth and just before diagnosis, they were huge, irritated and bleeding. If you have ever had these sores before, you know just how painful they can become. They can be found on the gums, inside the cheeks or lips, and on the tongue, and can last for up to 7-14 days.
Research has shown that people with celiac disease are more prone to developing aphthous ulcers (canker sores) then people without the disease. The numbers show that 16% of children and 26% of adults with celiac disease have recurring mouth sores, I can whole heartedly vote yes for this information as if I have been glutened, guaranteed, I will have canker sores develop in my mouth within a day or two.
As with other dental problems, malnutrition seems to be the culprit as to why people with celiac disease get these sores. Low levels of iron, folate and B12 could cause the sores to develop.
However, with that being said, there are a lot of reasons why canker sores develop in the mouth such as irritation being one of them. If you are concerned, consult with a doctor or a dentist as to the reasons you are getting them, it may not be that you are an undiagnosed case of celiac disease. Always consult with your healthcare professionals before you start making assumptions. - Dry Mouth
This is a condition that I have spoken about in another recent blog of mine that you can find here.
Having a dry mouth can result in tooth decay, the teeth need the saliva to stay healthy, which is why if you are a mouth breather you need to correct the biomechanics of this and become a nose breather. Saliva controls the bacteria that can develop in the mouth, so if it is not readily available, this can sometimes result in catastrophic tooth decay or tooth loss.
There is a condition called: Sjögren’s syndrome, which is an autoimmune disease that causes dry eyes and mouth because it attacks the glands you need for moisture of the mouth and eyes. Just because you have celiac disease does not mean you will develop Sjögren’s syndrome and vice versa.
Nonetheless, if you’ve been diagnosed with celiac disease and you suffer from dry mouth or dry eyes, you should talk with your doctor about the possibility of Sjögren’s syndrome. If it turns out you have both, prescription medicines are available that can help stimulate the flow of saliva and protect your teeth. - Inflamed Gums
This is another personal symptom of my own, every appointment at the dentist I am told that my teeth look fantastic (thank goodness), but my gums are always inflamed without any signs of plaque build up. Just before I was diagnosed with celiac disease my gums would bleed every time I brushed my teeth, I was later told that this can be a sign of malnutrition in the body.
I have been told my swollen gums could be due to the inflammation caused in my gut from the celiac disease damage that is still trying to heal and therefore could possibly be causing a chronic inflammatory response elsewhere in my body like my gums.
People with gluten allergies often suffer from periodontal disease and have inflamed, red, swollen, painful gums. A gluten-free diet can relieve the symptoms of gum disease by relieving inflammation. - Cheilosis
Cheilosis (also called cheilitis) is a painful inflammation and cracking of the corners of the mouth. It sometimes occurs on only one side of the mouth, but usually involves both sides.
This can occur in someone with celiac disease due to malnutrition and deficiencies in Vitamin B and Folate. It can also be related to megaloblastic anemia which is caused when red blood cells are not produced properly and the bone marrow produces abnormally large red blood cells.
This is another symptom that I personally have had when I was a kid and sometimes as an adult. This can be very painful and irritating as anything that touches it burns or every time you open your mouth, can rip it more. - TMJ Disorders
This is a condition that can be occurring due to an inflammatory response in the body from an autoimmune disease, an injury directly to your jaw, or it can be due to bruxism (a condition where you clench and grind your teeth).
Regardless of the cause, there is more research coming out that connects TMJ pain to celiac disease and the autoimmune response that occurs in the body because of it. More research needs to be done, but there have been connections of celiac disease and muscle and joint pain as well. - Thrush
This is a candida overgrowth within the body which is a fungus that includes over 20 species of yeast. This overgrowth can be common in people who are immune compressed and indicates a damaged immune system.
Once again, this is another symptom that I regularly delt with at first. This is also a condition that should have a blog post all to itself as there is a lot of information and research on this. - Plastic
This is not a symptom as it is something to be aware of. This absolutely blew my mind when I read about this as I use an orthodontic retainer every night. The plastic found in dental equipment or retainers could possibly contain a plastic called: plasticized methacrylate polymer. This is an additive to some plastics and contains gluten.
Back in 2013 there was a 9 year old girl diagnosed with celiac disease, who continued to be symptomatic even after eating a gluten free diet. Doctors eventually discovered that the orthodontic appliance she was using had the plastic additive mentioned above. After stopping use of the retainer, her symptoms improved and eventually she became symptom free. This just goes to show that it is not just what your consume but also what you use that could possibly have an effect on a celiac’s body. Be sure to check your toothpaste, mouth wash and lip chap for any gluten additives.
If you are concerned of any symptoms you may be experiencing, be sure to always consult your healthcare professional for more information.
References:
https://www.verywellhealth.com/effects-of-celiac-disease-on-dental-health-4115330
https://www.ncbi.nlm.nih.gov/pubmed/21507289
https://glutenfreern.com/dental-issues-and-celiac-disease-ep039/
https://www.ncbi.nlm.nih.gov/pubmed/24137038
https://glutenfreern.com/dental-issues-and-celiac-disease-ep039/
https://celiac.org/about-celiac-disease/related-conditions/oral-health/
https://www.colgateprofessional.com/education/patient-education/topics/other-issues/cheilosis
Please Keep This Disclaimer in Mind:
Articles are for educational purposes only and are not intended to diagnose, treat, cure or prevent diseases. We cannot and do not provide medical advice or specific advice on products related to treatments of a disease or illness.
You must not rely on the information on our website as an alternative to medical advice from your doctor or other professional healthcare providers.
You should never delay seeking medical advice, disregard medical advice or discontinue medical treatment because of information on our website.
It is your responsibility to consult with your professional health care providers before starting any diet changes, exercise or supplementation program, and before taking; varying the dosage and / or ceasing to take any medication.
We do not collect any personal information or store cookies. You can turn off cookies on your web browsers.